Key Takeaways:
- Traditional inert and bioabsorbable orthopedic implants demonstrate several drawbacks, including inflammation or infection, often requiring follow-up surgeries.
- A biointegrative, mineral fiber-reinforced polymer bone plate, designed to overcome these drawbacks, was implanted in sheep tibiae as part of a 2.5-year study.
- The plate demonstrated complete bioabsorption, with no adverse reactions, and left no trace of remnant material at the final study timepoint.
Current orthopedic implants for repairing fractures and bone deformities rely on either inert material that remains in situ or bioabsorbable material intended to break down and be cleared from the body. However, inert implants carry risks such as migration and chronic inflammation, while bioabsorbable implants have the potential to leave debris particles or absorb faster than the body can clear metabolites produced by the degradation process. Both implant types can therefore lead to complications requiring additional surgery.
Biointegrative, mineral fiber-reinforced bone fixation implants were designed to address the shortcomings of traditional bone repair materials through paced absorption that leaves no trace of residual debris or excess metabolites, while achieving full restoration of the native bone anatomy. A team led by Nicolette D. Jackson, DVM, MS, DACVP, Director of Medical Device Pathology at Inotiv, recently reported on this material in the Journal of Orthopaedic Research. During the course of a 2.5-year study conducted in sheep, the feasibility, safety, and biocompatibility of biointegrative fiber‐reinforced plates was demonstrated, showing that it holds promise as a new method for bone repair with no adverse events noted in the study.
Limitations Of Traditional Bone Repair Implants
Most bone repair implants are made from inert metals, which offer the advantages of strength, durability, low cost, and ease of insertion. However, these implants are not without risk and include adverse events like implant migration, bone tissue loss, infection, inflammation, local irritation, and even refracturing due to forces exerted by the implant.1 These issues can necessitate removal of the hardware, which carries its own set of potential complications.2
Bioabsorbable orthopedic implants attempt to avoid the drawbacks of metal implants by degrading in place, and therefore offer better general biocompatibility.3 However, remaining debris and metabolites produced during the degradation process can lead to foreign body reaction and subsequently to cysts, sequestra, or abscesses.4 Additional surgery may then be required to remove nonabsorbed polymer particles and inflammation-inducing products.4
To overcome these limitations, biointegrative, mineral fiber-reinforced bone fixation implants are designed to exhibit paced absorption. Because the material degrades in a gradual, progressive manner, it promotes an enhanced biointegrative response, leaving no permanent material which might require later surgical removal. The mineral components serve to promote bone regeneration and to balance acidic bioabsorption products, which can otherwise lead to acidic conditions in surrounding tissue and promote an inflammatory response.5,6 These implants have similar biomechanics to bone, a trait known to provide biofunctionality while promoting restoration of native bone anatomy.3
Study Design
In vivo plate implantation was conducted in a double-arm preclinical study, assessing the safety, biocompatibility, and biointegration of mineral-fiber reinforced plates. The implant was installed over the tibial bone surface in eight female sheep, a recognized model animal for testing bone repair methods, and tracked over the 134-week (2.5-year) study period using histology and microcomputed tomography (micro-CT).
The plate under study was a novel poly (L‐lactide‐co‐D, L‐lactide) (PLDLA) matrix reinforced with continuous mineral fibers composed of elements including calcium, silica, and magnesium, and organized into a layered structure oriented to provide optimal biomechanical properties. The implant material was approximately 50% mineral fibers and 50% polymer.
On the right tibia of each animal, the plate was implanted over the intact periosteum. On the left tibia of the same animals, the periosteum was elevated and retracted before plate implantation directly onto the bone cortical surface, simulating conditions that disrupt the periosteum.
Two animals were assessed at study weeks 13 and 26, and one animal each at 52, 78, 104, and 134 weeks.
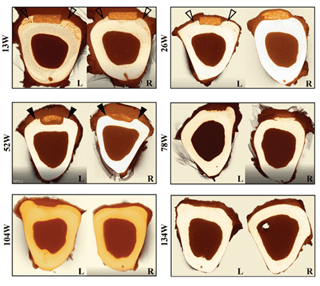
Fig 1. Micro-CT cross sections of sheep tibias with fiber-reinforced plates over cortical surface (left) and over intact periosteum (right). Over the course of the study, implant is absorbed and new bone growth is evident within the space previously occupied.
Tibial implant sites were collected and fixed for micro-CT and histopathology analyses. Histopathology findings were similar in both test arms, with no signs of inflammation in any animal, at any timepoint. Infiltration of anti-inflammatory M2-like macrophages and other indicators of bioabsorption, such as the presence of multinucleated giant cells, were observed in all animals, at all timepoints, with this positive response peaking at 52-78 weeks.
Bioabsorption was observed at the earliest timepoint, week 13, and peaked at 52-78 weeks. By week 104, only residual polymers were present, constituting approximately 5% of the implant area. At week 134, polymer was entirely absent, few macrophages were present, and no adverse tissue reaction was observed. No necrosis, hemorrhage, or foreign debris were present at any time point, in either study arm.
A Promising New Class Of Orthopedic Hardware
 The performance demonstrated by this study, conducted by Dr. Jackson and her team, provides an encouraging glimpse at the potential for fiber-reinforced implants to treat bone fractures and deformities in human patients. The implants achieved complete bone remodeling and total biointegration with no adverse tissue response. The versatility of the material was especially notable, showing similar positive results when simulating a minimally invasive surgical procedure or surgical treatment of severe bone trauma.
The performance demonstrated by this study, conducted by Dr. Jackson and her team, provides an encouraging glimpse at the potential for fiber-reinforced implants to treat bone fractures and deformities in human patients. The implants achieved complete bone remodeling and total biointegration with no adverse tissue response. The versatility of the material was especially notable, showing similar positive results when simulating a minimally invasive surgical procedure or surgical treatment of severe bone trauma.
This newly developed technology, now demonstrated to be feasible, effective, safe, and adaptable, provides a glimpse into a new class of orthopedic hardware that promises to provide more effective bone reconstruction, with fewer side effects and follow-up surgeries. In the future, the fiber-reinforced biointegrative plate may transform the treatment of orthopedic conditions, whether minor or severe.
References
- Page, S. M. & Stern, P. J. Complications and range of motion following plate fixation of metacarpal and phalangeal fractures. J Hand Surg Am 23, 827–832 (1998).
- Botte, M. J. et al. Complications of Smooth Pin Fixation of Fractures and Dislocations in the Hand and Wrist. Clinical Orthopaedics and Related Research 276, 194–201 (1992).
- Malekani, J., Schmutz, B., Gu, Y., Schuetz, M. & Yarlagadda, P. Biomaterials in orthopedic bone plates: a review. in Proceedings of the Annual International Conference on Materials Science, Metal and Manufacturing 71–76 (Global Science and Technology Forum, 2011).
- Choi, S. H. & Lee, J. H. Absorbable Plate-Related Infection after Facial Bone Fracture Reduction. Arch Craniofac Surg 17, 1–4 (2016).
- Rreiss‐Bloom OPD, Merchav‐Feurmann R & Lindner T. OSSIOfiber(TM) intelligent bone regeneration technology overview. https://resources. ossio.io/white-paper-on-the-ossiofiber-technology (2019).
- Verrier, S., Blaker, J. J., Maquet, V., Hench, L. L. & Boccaccini, A. R. PDLLA/Bioglass® composites for soft-tissue and hard-tissue engineering: an in vitro cell biology assessment. Biomaterials 25, 3013–3021 (2004)
From:
- Jackson, N. D., Nyska, A., Palmanovich, E. & Nyska, M. The biointegration profile of fiber‐reinforced plates following tibial implantation in sheep. Journal of Orthopaedic Research (2023) doi:10.1002/jor.25682.



